We’ve all heard the claim that red meat increases the risk of colon cancer. Leaving aside the totally ridiculous nonsense (“meat rots for 5 years in your colon” – no, it doesn’t.), it’s reasonably clear that there’s an association between red meat consumption and colon cancer risk. But an association only points to the potential existence of a cause; it doesn’t actually prove that any causal relationship exists.
Of course, there are proposed explanations for why red meat supposedly contributes to colon cancer, most notably the iron in the red meat. But if you dig deeper into the reasons, things stop adding up quite so well. The real story might be less “red meat” and more “red meat in the context of a lousy diet” – which of course is how most Americans eat their red meat. Here’s a look at the connection between iron from red meat and colorectal cancer, and how that breaks down when you look closely.
Red Meat, Iron, and Cancer
So why does red meat supposedly cause cancer? It’s not the fat: meat fat doesn’t make any significant contribution to colon cancer. It’s also not cooking by-products (the potential carcinogens that form when you cook meat at high temperatures).
Iron is much bigger of an issue than either of those two. And the problem is specifically heme iron, the type of iron found in meat. There are basically two types of dietary iron: heme iron and non-heme iron.
- Heme iron: found in animal foods, like red meat and seafood.
- Pro: more easily absorbable and usable for the human digestive system, so it’s a much more effective way to get iron from your mouth into your body.
- Con: may increase colon cancer risk. (Hold that thought for a minute)
- Non-heme iron: found in vegetable foods, like spinach and chickpeas.
- Pro: not associated with colon cancer risk.
- Con: not very absorbable (one reason why many vegans are iron-deficient despite eating a lot of spinach)
This study goes into a long explanation of how heme iron is a trigger for oxidizing fats, and the evidence that heme iron is much more significant than other potentially carcinogenic aspects of red meat.
Without getting into too much detail: heme iron triggers a process called lipid peroxidation (basically damage to fats in the colon), and the result is an environment more toxic to normal cells than to potentially cancerous cells. This allows potentially cancerous cells to thrive at the expense of normal cells, increasing cancer risk. Scientists can measure this by measuring byproducts of lipid peroxidation in urine.
So now we have an issue: iron deficiency is one of the few remaining widespread nutrient deficiencies in the US (especially among premenstrual women and people with malabsorptive digestive disorders), and yet we’re supposed to avoid our best dietary source of iron for fear of getting colon cancer? What gives?
Before you worry, keep reading.
Fat Oxidation and PUFA Consumption
Heme iron causes damage by oxidizing fats. But not all fats are equally easy to oxidize. Paleo veterans, you get three guesses about the villains here, and the first two don’t count.
No idea? The most easily oxidizable fats in the human diet are…polyunsaturated fats! Polyunsaturated fats (PUFA for short) were relatively rare in our evolutionary diet, but as peanut and soybean oil started replacing lard and tallow, and as we started eating more and more fried junk food, they’ve been making up more and more of the typical American’s daily calorie intake.
There are two types of PUFA: Omega-3 and Omega-6. If you don’t know the difference, here's a quick refresher:
- Omega-3: Found in fish and seafood; associated with better cardiovascular and mental health; anti-inflammatory. Our consumption of Omega-3 has declined over the years, even though our total PUFA consumption has gone up, thanks to…
- Omega-6: Found in industrial oils, nuts, seeds, and to a lesser extent pork and poultry. These fats are much more inflammatory and responsible for driving the total PUFA increase.
The increase in PUFA in the American diet has been mostly Omega-6 PUFA. Today we eat too much total PUFA and way too much Omega-6, but ironically most people actually aren’t getting enough Omega-3. We’re just getting such an incredible Omega-6 overload that our total PUFA consumption is still too high.
That’s kind of a complicated problem. Here’s a diagram to break it down a little differently:
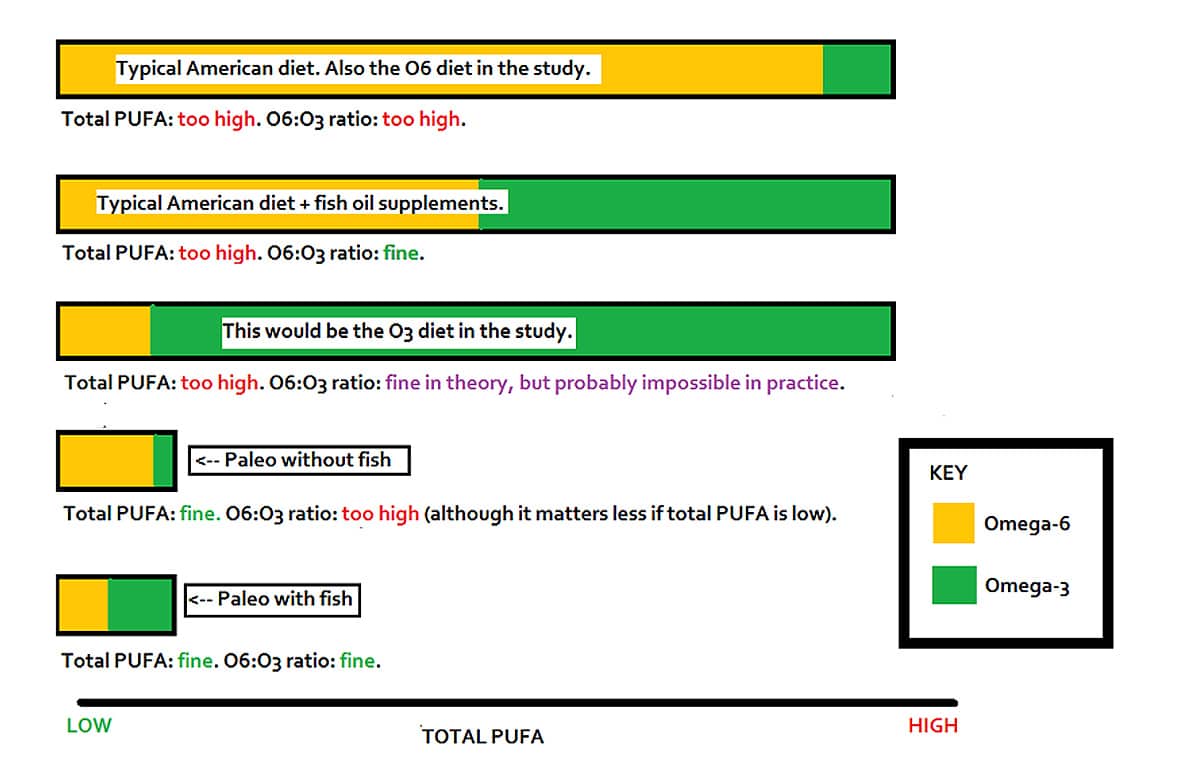
OK, back to the problem of iron and colon cancer. The heme iron found in meat, the reason why meat supposedly contributes to colon cancer? It might only be a problem in the context of a high-PUFA diet. That would be the top three bars on the diagram above.
This study goes into detail about an experiment (admittedly in rats, but that’s also where most of the red meat experiments come from, so call it fair). The researchers gave the rats one of three diets:
- High in heme iron, but low in PUFA (fats from coconut oil, which is almost exclusively saturated fat)
- High in heme iron, and high in Omega-6 PUFA (safflower oil)
- High in heme iron, and high in Omega-3 PUFA (fish oil)
Heme iron + coconut oil had almost no effect on markers of lipid peroxidation. The supposedly evil heme iron didn’t really do anything when you combined it with the (also supposedly evil) saturated fat. But both forms of PUFA dramatically increased markers of lipid peroxidation, when combined with dietary heme iron. The authors suggested that the biomarkers were formed by oxidation of the PUFA during digestion.
The study also noted took fecal extracts from the rats. When the extracts were applied to the colon cells, heme iron + PUFA extracts did by far the most damage. That suggests that the real danger is adding heme iron to a high-PUFA diet, not just heme iron on its own.
The authors concluded by suggesting that “control of …dietary intake [of PUFAs] is needed also because of their pro-inflammatory, toxic, and even cocarcinogenic effects.”
What does That Look Like in Food?
The “dangers” of heme iron depend on a high PUFA intake, either Omega-3 or Omega-6. So the goal is to have a low total amount of PUFA, with a balanced ratio of Omega-6 to Omega-3, preferably between 4:1 and 1:1. If you translate that into actual food recommendations, here’s what you get:
- Avoid PUFA-rich seed oils. Soybean oil, peanut oil, safflower oil. You’d want to avoid these guys even if you didn’t have a colon at all: they do more than just contribute to colon cancer.
- Eat fatty cold-water fish regularly. Wild-caught salmon and sardines are good choices. Don’t take a fish oil supplement unless your doctor specifically recommends it.

Some other studies also suggest various other strategies for reducing any potential heme iron toxicity and reducing colon cancer risk in general:
- Eat plenty of calcium, from leafy green vegetables, bone-in fish, and dairy sources if you tolerate them well. Calcium may help reduce heme iron toxicity.
- Eat green leafy vegetables for the chlorophyll, which might also protect against heme problems.
- Eat fibrous vegetables to your personal tolerance; they encourage your gut bacteria to make anti-inflammatory fats that protect against colon cancer.
- Eat some coconut oil! As well as being a “safe fat” in the study discussed above, in one study, the fats in coconut oil specifically helped protect against colon cancer.
That pretty much jives with the basic Paleo template: some meat, lots of vegetables in different colors, and healthy fats.
Summing it Up
It’s not surprising that red meat is associated with colon cancer in the general population: “red meat” is typically code for “eats a lot of junk,” and that junk often involves a lot of PUFA.
Eating red meat in the context of a high-PUFA diet might very well increase oxidative damage in the colon and the risk of colon cancer. But if you take out one of those two factors, then it’s not actually clear how well the link holds up. If you wanted to eliminate either heme iron or PUFA…
- You could take out red meat, which provides all kinds of other important vitamins and minerals, high-quality protein, and healthy fats.
- Or you could take out the industrial oils, which don’t provide any vitamins or minerals. And on top of reacting with heme iron, they also irritate the lining of the gut and cause inflammation in various other ways.
From a Paleo perspective, the choice is pretty clear!





Leave a Reply